PHONE US: (778) 484 1484
What is gingivitis?
March 8, 2017
Gingivitis and gum disease are often used interchangeably, but the terms actually refer to two stages of periodontitis disease.
When you think of oral health, what comes to mind? For most of us, it would include brushing and flossing to prevent cavities. However, one's oral health includes more than just the teeth. The structures that hold your teeth in place, or you gums, are just as important as those pearly whites.
What is gingivitis?
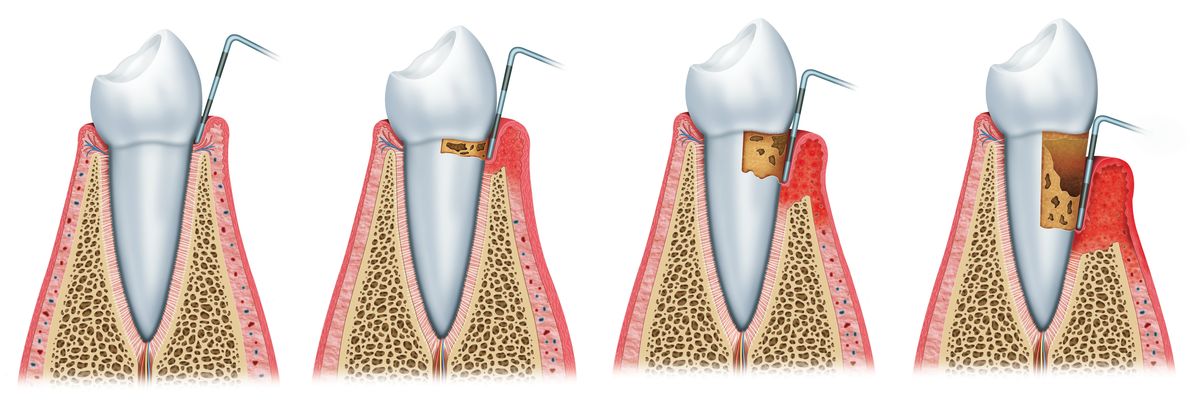
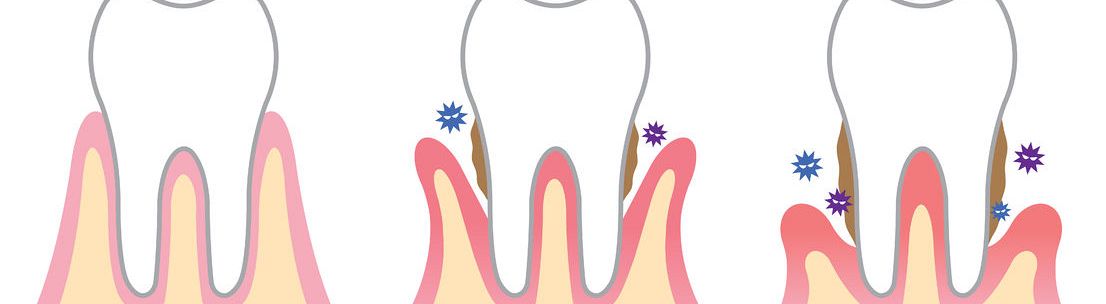
The word gingivitis refers to the inflammation of the gums, which can show up as swollen, red, and irritated. It is a mild form of gum disease, one that can be reversed with proper care.
The most common cause of gingivitis is a bacterial infection, a result of the buildup of plaque on the teeth, which is a non-destructive type of periodontal disease. Where the gum meets the tooth is not actually where it attaches, creating a small space that food can become trapped in. When plaque eventually develops and extends below this gum line, it can cause gingivitis.
What is gum disease?
If left untreated, over time gingivitis can advance to periodontitis or gum disease. In this instance, the gum will pull away from the tooth, form a pocket, and become infected. As the body fights the infection, the tooth can begin to loosen and will eventually have to be removed if not treated.
Symptoms of gingivitis and gum disease
The symptoms of gingivitis and gum disease can overlap, and vary in severity depending on the person. Some of the symptoms include:
-
Red or swollen gums
-
Bleeding gums (especially after brushing or flossing)
-
Bad breath
-
Loose teeth
-
Receding gums (teeth will appear longer)
-
Sensitive or painful teeth
Any of these symptoms should not go unchecked, and require an appointment with your dentist. In many cases it can be reversed, so the sooner you see a professional, the more chance there is to control the infection and take steps to prevent it occurring again.
Why do my teeth hurt when I eat cold foods?October 3, 2018
We all like to enjoy a nice, refreshing beverage or a bite of ice cream now and then. But, if you feel a sudden jolt of pain in your teeth and gums when you do, you ma...
Read MoreDo your gums bleed?September 25, 2018
When we talk about oral health, it’s important not to forget the gums. Unlike teeth, gums are made of soft, delicate tissues that can become irritated fairly eas...
Read MoreHow do I know if I need a root canal?August 30, 2018
If you have a tooth that is severely damaged, a root canal may be the option to save the tooth and restore your dental health. Infections in the ro...
Read More